Headache & migraine
In OTC
Follow this topic
Bookmark
Record learning outcomes
Which? showed that pharmacy staff are not offering adequate advice. So how can they get ahead?

Â
Learning objectives
After reading this feature you should be able to:
- Recognise the different types of common headache
- Accurately identify migraine
- Recommend the most appropriate treatments and offer self-care advice for migraine and headache
Â
Most headaches, including migraine, although debilitating for the sufferer, aren’t serious and can be treated with OTC remedies and self-care.
However the recent Which? report found that nearly a quarter of pharmacy staff, in particular medicine counter assistants, were unsure about the sales procedure for OTC sumatriptan (Imigran Recovery) and the advice they should be offering migraine sufferers. In some cases the mystery shoppers, posing as ideal candidates for the medication, were unnecessarily referred to their GP.
Other research shows that migraine is under-diagnosed and under-treated in at least half of patients and that one-third of sufferers will experience significant disability as a result of their migraines at some stage of their lives. Such research demonstrates how crucial it is that pharmacy staff understand the type of headache a customer has and the best treatment to recommend.
“The pharmacy team needs to be able to feel confident about recommending migraine treatments based on what is best for the patient,†says community pharmacist Sultan Dajani. “If they are unsure, then this is something they should do as a CPD point. Having Imigran Recovery as an OTC medication and not using it is a waste for patients in terms of their quality of life – and it is also a waste of a POM to P switch.â€
While there are around 200 distinct types of headache, 95 per cent are due to four types of treatable disorders:
- Tension-type headache
- Migraine
- Cluster headache
- Medication overuse headache.
These types of headaches are known as primary headaches (i.e. they are based on symptoms and are not due to an underlying health problem).
Another category is secondary headaches (i.e. those headaches that have a distinct cause). This category includes headaches associated with a head injury, stroke, substance misuse and/or its withdrawal (including alcohol), infection and disorders of the neck, eyes, nose, sinuses or teeth.
 Migraine is under-diagnosed and under-treated in at least half of patients
Dr Mark Weatherall, consultant neurologist at Charing Cross and Ealing Hospitals and a trustee of the Migraine Trust, says: “Primary headache disorders are by far the commonest type of headache. If you start from the basis that patients are sufficiently troubled to actually seek advice about their headache rather than just take tablets at home, then the most likely reason that they are seeking advice in the pharmacy is that they have a migraine.â€
Migraine affects 8 million people in the UK, mostly adults aged 35-45 years, but it can affect all ages including children. Migraine is commoner in women – affecting 18 per cent of women compared to just 8 per cent of men.
How to identify migraine
Migraines are experienced as a headache of at least moderate severity, usually on one side of the head, accompanied by other symptoms such as nausea, vomiting, and sensitivity to light and noise. The headache is usually made worse by physical activity. Migraines usually last from four to 72 hours and in most cases there is complete freedom from symptoms between attacks.
Certain factors are involved in triggering an attack in those pre- disposed to migraine. These can include lifestyle and hormonal changes.
There are several types of migraine:
• Migraine with aura is when there is a warning sign before the migraine begins. About a third of people with migraine have this. Warning signs may include visual problems (such as flashing lights) and stiffness in the neck, shoulders or limbs
• Migraine without aura
• Migraine without headache, also known as silent migraine. This is when an aura or other migraine symptoms are experienced, but a headache does not develop.
Episodic migraine (defined as fewer than 15 headache days a month) is the commonest migrainous condition and can occur at any time. Frequency can vary between one attack a year to one a week.
Chronic migraine is defined as more than 15 headache days a month over a three-month period, of which more than eight are migrainous. Those afflicted are classified as chronic sufferers. This type of migraine affects less than 1 per cent of the population.
About a third of people who suffer with migraine have aura
The most basic way to diagnose migraine is to identify a recurrent headache with certain features. Migraine should comprise:
- At least two of the following symptoms: unilateral pain, throbbing pain, aggravation by movement, moderate or severe intensity
- At least one of the following symptoms: nausea/vomiting or photophobia and phonophobia.
A pharmacist can make a migraine diagnosis if the patient has an established pattern of migraine.
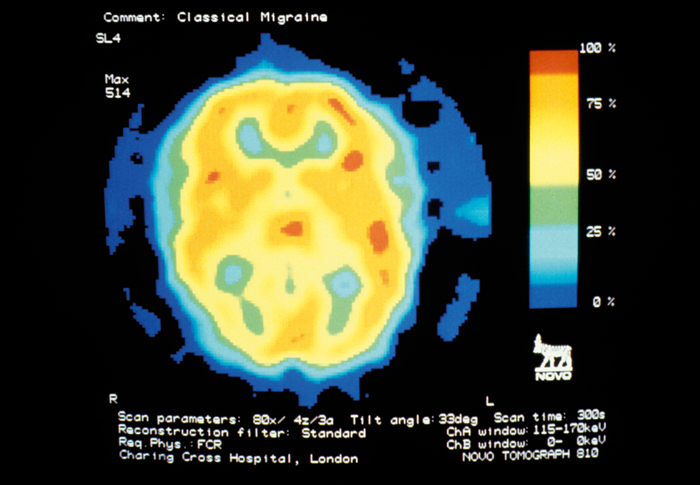
Single photon emission tomography image of the brain in a patient during an attack of classical migraine.
Migraine treatments
The main non-prescription migraine treatment options are analgesics and sumatriptan.
Analgesics
Analgesics, such as paracetamol, NSAIDs (aspirin, ibuprofen and diclofenac) and combined analgesics containing paracetamol or an NSAID with codeine, can be used as first-line treatment to relieve the pain of the migraine headache. There are also treatments that can be combined with paracetamol, such as buclizine and prochlorperazine to treat the nausea as well as the headache.
If the patient is nauseous a soluble painkiller may be recommended as these are absorbed quicker from the stomach.
When to recommend analgesics
Analgesics can be recommended:
- For the first three attacks of migraine unless the initial attacks are very severe and disabling
- If the customer has previously used analgesics and is happy with the relief they provide
- For customers who have not been diagnosed with migraine.
When not to recommend analgesics
Analgesics should not be recommended:
- If the treatment has failed on three occasions
- If a woman is pregnant (refer to doctor)
- Refer to doctor and do not give NSAIDs to a customer who has ulcers or a history of bleeding in the stomach or intestines, anaemia, high blood pressure, or kidney, liver or heart disease
- Be cautious when recommending NSAIDs to asthmatics
- Be alert to a patient who might be chronically overusing analgesics or addicted to their properties and consequently suffering from medication overuse headache.
“The first general principle for migraine is to recommend that patients take an [appropriate] dose of whatever painkiller they are going to take as early as possible when they feel an attack coming on,†says Mark Weatherall. “People sometimes have a tendency to take, say, 500mg of paracetamol two hours into an attack and will then get only a mild or partial response.
“With simple analgesics, that means taking paracetamol 1g or [the maximum dose of] ibuprofen. People should not take more than 1,200mg ibuprofen in a day or 900-1,200mg of aspirin a day. As well as advising on an adequate dosage of analgesics, the pharmacist should also ask questions about nausea and, if needed, recommend an anti-emetic.
“Although medication containing codeine is widely advertised and available for treating migraine I would always advise pharmacists to be cautious about recommending opiates because there is quite a high chance of people becoming dependent on them or developing medication overuse headache. I spend a lot of my working life getting people off codeine.â€
Triptans
Triptans (e.g. sumatriptan) are generally recommended to sufferers if ordinary painkillers are not helping to relieve their migraine. They relieve pain by narrowing blood vessels in the head and blocking the transmission of pain in the sensory nerves that supply the skin and structures of the face. As well as relieving the pain associated with migraine, sumatriptan also relieves nausea and sensitivity to light.
The OTC triptan Imigran Recovery (sumatriptan) has replaced its pre-sale two-page questionnaire with a simpler sales protocol that can be used as a reference for pharmacy staff.
When to recommend sumatriptan
Sumatriptan can be recommended:
- For customers with an established and stable pattern of migraine
- For customers who have failed to obtain relief from OTC analgesics on three occasions
- If the initial attacks are very severe and disabling.
When not to recommend sumatriptan
Sumatriptan should not be recommended to:
- Those under 18 or over 65 years of age
- Pregnant or breastfeeding women (refer to doctor)
- Customers with heart problems or with a family history of heart problems
- Customers who have had a stroke
- Customers with high blood pressure
- Customers with kidney, peripheral vascular or liver disease
- Customers with epilepsy or who are prone to fits
- Women taking combined oral contraceptives (refer to GP).
When to refer...
Red flag symptoms associated with headache include:
- Frequent or severe headaches that come on suddenly
- Anyone complaining of the following symptoms: unilateral muscle weakness, double vision, tinnitus, clumsy and uncoordinated movement and reduced level of consciousness, weakness of muscles controlling eye movement, along with a headache lasting a week or more
- A headache following an accident, in particular a head or neck injury
- Anyone experiencing blackouts
- Headaches brought on with every cough, sneeze, bend or by standing up
- Weakness, numbness or slurred speech
- Anyone with a headache lasting longer than 24 hours
- Additional features such as seizure-like movements, a rash or a headache confined to the back of the head
- Headaches that frequently wake someone from sleep
- Anyone whose migraine attack occurs for the first time after 50 years of age
- Anyone diagnosed with high blood pressure
- Recent marked deterioration in migraine (duration, severity or frequency)
- Women with migraine using the combined oral contraceptive pill.
Â
“If a customer has been previously diagnosed with migraine and in the absence of any other neuro symptoms or injury I would have no qualms about recommending sumatriptan as a first-line treatment because taking other painkillers might just be delaying the inevitable,†says Sultan Dajani. “It is a perfectly safe medication, the side-effects are very rare and the worst case scenario is that it won’t work. If that is the case, then it’s a sign the patient needs to see their GP.â€
Migraine and self-care
Pharmacists have a key role to play in educating migraine sufferers on how to bring their condition under control and take preventive action between attacks to help avoid migraine altogether.
Triggers for migraine attacks can vary from one person to another and sufferers should be advised to keep a migraine diary to try to identify the causes. It is likely a combination of triggers will cause a migraine attack.
Triggers can include:
- Certain foods (e.g. cheese and chocolate) and drinks containing caffeine and alcohol
- Emotional stress
- Menstrual periods
- Changes in normal sleep pattern
- Extreme fatigue
- Skipping meals and fasting
- Sudden changing weather conditions
- Exercise
- Smoking
- Bright and flickering lights
- Odours
- Medicines such as the combined oral contraceptive pill, hormone replacement therapies and sleeping tablets.
Migraine diary
A migraine diary should record:
- When the migraine started and ended
- The symptoms
- Whether it’s a throbbing or piercing pain
- Where the pain is
- Any other medication taken prior to the attack
- Amount of sleep prior to the attack
- Food eaten recently
- Any recent exercise.
“Migraine is a complex disorder with very individual symptoms and triggers,†says Dr Nicholas Silver, consultant neurologist at the Walton Centre, Liverpool. “That’s why it is important for sufferers to understand their condition and what triggers attacks so they can get the best out of their healthcare professional. The most successful migraine management plans rely on a foundation of good lifestyle and effective treatment.â€
Commonest types of recurring headache
Tension headache
Tension-type headaches are the most commonly occurring. The pain is often described as feeling like a tight band around the head or a weight on top of it. The neck or shoulder muscles may also hurt and the pain can last from 30 minutes to several days, or may be continuous.
Stress is one cause, but others may include drinking too much alcohol, not getting enough sleep, depression, skipping meals and becoming dehydrated.
Whereas migraine can be identified as a headache with associated features, such as nausea and sensitivity to light, people experiencing headaches without features are likely to be suffering from the tension variety.
These headaches can be treated with OTC painkillers such as ibuprofen and paracetamol. Self-care advice could include learning relaxation techniques, avoiding stressful situations where possible, using hot and cold packs to relax the muscles in the head and neck, or massaging the affected areas.
Cluster headache
Cluster headaches are one of the most painful conditions an individual can experience and are even more debilitating than migraine. They are excruciatingly painful headaches, which cause an intense pain around one eye. A relatively rare condition affecting one or two people in every 1,000, cluster headaches are often misdiagnosed as migraine or sinus headache and subsequently mistreated.
With cluster headaches the pain is always unilateral and, although for some people the side can vary from time to time, it is usually centred over one eye, one temple or the forehead. It can spread to a larger area making diagnosis harder. Cluster headaches occur in clusters for four to 12 weeks around the same time of year. The pain is often experienced at a similar time each day. Such patients should be referred to the GP.
Medication overuse headache
Medication-induced headache, the third commonest cause of headache, is the result of taking painkillers too often. Up to one in 50 people experience headaches caused by medication overuse and women are five times more likely to get them than men.
NICE guidance advises pharmacists to be alert to the possibility of medication overuse headaches in people whose headache developed or worsened while they were taking the following drugs for three months or more:
- Triptans, opioids, ergots or combination analgesic medications on 10 days a month or more
- Paracetamol, aspirin and a NSAID, either alone or any combination, on 15 days a month or more.
Such patients should be referred to the GP.
Martin Underwood, a GP and professor of primary care research at Warwick Medical School, who chaired the NICE guideline on the diagnosis and management of headache, says: “Treatment involves stopping medication abruptly with the headache getting much worse for several weeks before it will improve. When talking to people about a headache it is important to warn them to prevent medication overuse.â€
Key facts
- Migraine affects 8m people in the UK
- Some pharmacy staff lack confidence when it comes to recommending sumatriptan
- People who take painkillers on a regular basis are at risk of developing medication overuse headache.
Â
